The University of Limerick School of Medicine was established in 2007 and, two years later, the first cohort of 32 students went on an 18-week LIC in general practice. Currently, we have approximately 200 students undertaking the LIC each year. We are an enthusiastic and ambitious group of GP teachers and researchers aiming to develop general practice and primary care in Ireland with high quality teaching and research of international standing while maintaining active clinical roles and involvement in the development and delivery of primary care services in the Mid-West and beyond. We deliver an innovative educational programme at the School of Medicine where we teach in three of the four years of the graduate entry medical programme. The Early Patient Contact Programme is based entirely in general practice and our 18 week Longitudinal Integrated Clerkship placement programme in the community is unique in Ireland. This programme is consistently rated highest of all clinical placements by medical students here at UL. In addition, we deliver interdisciplinary postgraduate education and have created a highly supportive environment for our postgraduate students.
We are proud of the fact that our research impacts not only on individual patient care but also on regional and national health policy: The Limerick Declaration on Rural Healthcare 2022 https://www.rrh.org.au/journal/article/7905.
We have a highly successful funding and publication track record nationally and internationally and have numerous research awards including:
- the Fáilte Ireland Social Impact & Legacy 2023 award for the WONCA 2022 World Rural Health Conference https://www.failteireland.ie/Utility/News-Library/failte-ireland-honours-conference-ambassadors.aspx
- Irish Healthcare Awards 2023 ‘Patient organisation of the year award category' for 'Dancing for pulmonary fibrosis' research project (ILFA - Irish Lung Fibrosis Association)
- Royal Academy of Medicine 2023 Award in the General Practice category, The evaluation of a training course to enhance intellectual disabilities and mental health awareness amongst General Practitioners attending police stations.’ Irish Journal of Psychological Medicine https://doi.org/10.1017/ipm.2022.25
- ICGP best published paper in general practice 2022 award for 'How do multi-morbidity and polypharmacy affect general practice attendance and referral rates? A retrospective analysis of consultations. PloS One. 2022 Feb 3;17(2):e0263258 https://journals.plos.org/plosone/article?id=10.1371/journal.pone.0263258
We look forward to the opportunity to engage with you through all or some of the activities outlined above and above all else “Welcome to the School of Medicine!”
Professor Liam Glynn
MD, MICGP, FRCSI, FRCGP, FFSEM
Professor of General Practice
Head of Discipline
School of Medicine
Faculty & Staff
- Professor Liam Glynn - Professor of General Practice
- Professor Peter Hayes - Professor of Rural General Practice
- Professor Patrick O'Dwyer - Adjunct Clinical Professor of General Practice (BM4003 Module Lead)
- Professor Aidan Culhane - Adjunct Clinical Professor of General Practice (Early Patient Contact Programme Lead)
- Professor Róisín Doogue - Associate Professor of General Practice
- Dr Andrew O'Regan - Associate Professor of General Practice
- Dr Patrick O'Donnell - Associate Professor of General Practice
- Dr Sarah Hyde - Associate Professor of Clinical Education
- Dr Christine Kelly - Rural Fellow in General Practice
- Ms. Mary Fleming - Executive Administrator, General Practice
- VACANT - Senior Administrator, GP Education & Assessment
- Ms. Monica Casey - Senior Administrator, ULEARN-GP Network & Research
- Professor Pat O'Dwyer, Limerick/North Tipperary Co-ordinator, e-mail: patrick.odwyer@ul.ie
- Professor Aidan Culhane, Limerick/North Tipperary Co-ordinator, e-mail: aidan.culhane@ul.ie
- Dr Páraic Meaney, Clare Co-ordinator, e-mail: paraic.meaney@ul.ie
- Dr Declan Herlihy, Cork/South Tipperary Co-ordinator, e-mail: declan.j.herlihy@ul.ie
- Dr Ryan Say, Kerry Co-ordinator, e-mail: ryan.say@ul.ie
- Dr Noreen Lineen-Curtis, North West Co-ordinator, e-mail noreen.lineen-curtis@ul.ie
- Dr Jerry O'Flynn, Midlands Co-ordinator, e-mail: jeremiah.oflynn@ul.ie
- Dr John Cuddihy, South East Co-ordinator, e-mail: john.cuddihy@ul.ie
- Dr Stan Natin, Dublin Co-ordinator, e-mail: stan.natin@ul.ie
ULEARN-GP Network
The University of Limerick Education and Research Network in General Practice (ULEARN-GP) is a collaboration of approximately 150 general practices across the country. Our affiliation with these practices enables us to offer high quality placements to our students as well as to advance the research interests of the School, specifically in the areas of public health and primary healthcare. The network is sub-divided into eight geographic "hubs", each led by an individual GP Co-ordinator.
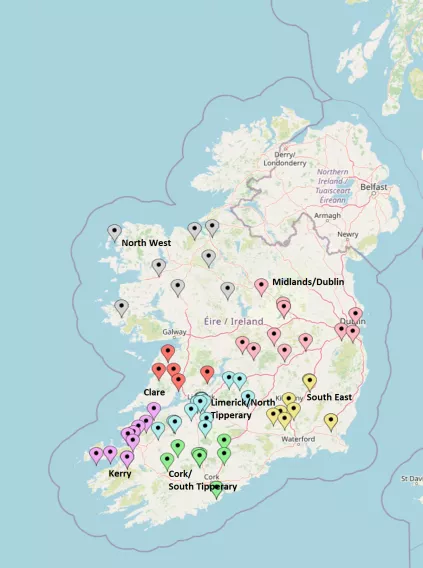
Overview of the General Practice/Primary Care Module
In Year 3, each student spends 18 weeks on clinical attachment with an individual GP tutor in a UL-affiliated teaching practice.
Currently, teaching practices are located in eight regions, each with a central hub at which students attends for the day release programme. During the initial part of the placement students observe the GP tutor consulting with patients. However, the core component of this clinical attachment is 'parallel consulting', where a patient is assigned to a student by the GP tutor (with the patient's consent). The student then consults with the patient for 15 to 20 minutes before presenting his/her findings to the GP tutor. While clinical responsibility for patient care will always rest with the GP, this model involves the student in the assessment and management of patients presenting to general practice and is therefore an 'active' form of learning.
Students, on average will encounter 4 to 6 patients per day, generating approximately 400 patient contacts over the 18 week placement. Students learn to perform the same tasks as the general practitioner, while under close supervision.
Teaching
Formal teaching takes place at one of the School’s regional teaching hubs on Wednesday mornings with 6-12 students per hub. This day release programme consists of seminars/webinars delivered by invited speakers and also a series of 5 small group tutorials, which are delivered by regional GP co-ordinators.
Activity in each of these eight networks is locally supported by a GP Co-ordinator whose primary role is to support practices and students and to liaise with UL and is thus your local point of contact in the event of issues arising from your placement.
Typical Student Schedule for GP Placement
|
|
Monday |
Tuesday |
Wednesday |
Thursday |
Friday |
|
AM |
GP Clinic |
GP Clinic |
Formal teaching in GP (block release) |
GP Clinic |
GP Clinic |
|
PM |
GP Clinic |
Self-directed learning |
Professional Competencies (block release) |
Self-directed learning |
Self-directed learning |
Frequently Asked Questions
Assessment of the module involves three domains, each contributing one-third to the overall score. Students must achieve a minimum of 50% in each of these domains to pass the module. The In-Training Assessment is completed by the student's clinical tutor on placement. The Knowledge of Health and Illness component is a written exam comprising multiple choice questions (MCQ) and extended matching questions (EMQ). The Long Case clinical exam is the final component where the student interviews/examines a patient and must then answer questions on their findings/diagnosis by an examiner pair.
During the early weeks of placement, the student will "sit-in" with the GP tutor simply as an observer. Soon after this, the student must start to actively consult with patients before presenting the case to the clinical tutor. This approach promotes "experimential learning". While clinical responsibility for patient care will always rest with the GP, the "parallel consulting" approach allows students to actively support this activity. The primary responsibility of the GP Tutor is to review the findings that have been presented/summarised by the student and to provide regular and constructive feedback to the student on his/her clinical history, examination and likely differential diagnosis. Secondary responsibilities include observing / reviewing the student’s ability to:
- Communicate with the patient
- Demonstrate a physical exam skill
- Discuss diagnosis / differential diagnosis
- Explain pathophysiology of the condition, investigations and management, relevant research in the area.
Students must attend all five of their small group tutorials throughout their 18-week placement. Students must also attend at least 75% of the "fixed teaching" sessions and workshop days.
No. To ensure the quality and transparency of the placement, students are allocated to a UL-approved practice that is unfamiliar to the student. All students are required to disclose upon receiving their allocation that they have never lived within 10km of their assigned practice (or 5km in the case of the large urban areas Dublin, Cork, Limerick, Waterford) and that none of their first degree relatives are employed by or are registered as patients at the practice. Students are, however, permitted to rank their preference of network regions 1-8 (see ULEARN-GP network above) where they wish to be placed in the pre-placement questionnaire.
'Career destinations of graduates from a medical school with an 18-week longitudinal integrated clerkship in general practice: a survey of alumni 6 to 8 years after graduation.' https://link.springer.com/article/10.1007/s11845-020-02260-0

Why am I a GP? A large part of it is due to my time in West Clare in early 2010 as a UL GEMS student. Days were filled with clinical encounters, parallel consultations, house calls, out of hours and immersion in local life which shaped my enthusiasm for GP life. GPs are perhaps the last of the generalists in medicine, and with my allocated practice being 80km from an ED, knowing your patients and good clinical skills were essential. GP is cradle to the grave medicine and no two days are the same. At times you are there just to listen or reassure. Other times it’s to break bad news or treat serious illness. As a career it can be demanding but ultimately personally rewarding.
Brian King
BMBS Class of 2011 Graduate and General Practitioner

I graduated from UL in 2022 and looking back, my general practice placement was such a great opportunity to get to know patients and see the impact of management plans over time. The placement allowed me to live in the beautiful Irish countryside for 18 weeks, with weekends spent sightseeing and exploring the Atlantic Way, having world-renowned beaches as my backyard. It was truly surreal, especially as an international medical student from Canada. There are always research opportunities as well - I had the chance to work with an outstanding research team on the Med-Well Programme, an initiative that changed the medical curriculum and is still in place today.
Aubree Worobetz
BMBS Class of 2018 Graduate
Internal Medicine, Canada